Child head injury: "My baby girl is back"
Hannah-Grace, her mother and aunt recently visited Dr Palesa Monyake and the multidisciplinary paediatric intensive care unit (PICU) team at Netcare Waterfall City Hospital.
Specialised care in Hannah-Grace’s triumph over tragedy
The medical care in the immediate aftermath of a head injury, combined with rehabilitation therapies in the weeks that follow, can make all the difference in the life of the survivor – particularly when a child’s future is at stake.
“We never thought something like this could happen. The accident came without warning. Another vehicle hit us at high speed. We were far from home, as we had been visiting friends in Mpumalanga,” recalls Megan Hefer, of Fochville, Gauteng.
Three and a half year old Hannah-Grace Hefer’s life hung in the balance following a tragic car accident in the first week of 2026 that cut short the life of her devoted father and left her mother, Megan, with an injured arm and a badly swollen eye.
“At the scene of the accident, Hannah-Grace’s eyes were fixed and unfocused: I knew that was a bad sign,” Megan recalls.
“Hannah-Grace was in such a bad way, we hardly dared to hope for the kind of recovery she has made,” recalls Dr Palesa Monyake, paediatric intensivist at Netcare Waterfall City Hospital’s specialised paediatric intensive care unit.
Yet, just two months after the accident, the little girl described as a ‘go-getter’ is returning to her lively, active self and surpassing everyone’s expectations for a recovery after brain injury.
“She was airlifted from Ermelo in a critical condition with severe head injuries, and when she arrived Hannah-Grace kept having seizures and could not even breathe on her own.”
“As a mother myself, I knew how difficult it must be for Mrs Hefer to be separated from her injured child without knowing who was looking after her. The next morning, I visited her in the hospital to introduce myself and promise her we would take care of Hannah-Grace just as if she were our own child,” Dr Monyake says.
After several days, Hannah-Grace’s condition slowly began to improve under the diligent care of doctors and paediatric intensive care unit nurses, whom Megan describes as ‘angels doing God’s work’.
“On 7 January, they extubated Hannah-Grace and I had to leave her in the hospital to identify my husband’s body. On the same day, I received two blessings. Firstly, Hannah-Grace woke up for the first time since the accident, and secondly, my sister safely delivered a healthy baby. There were so many emotions, but for me, it was the Lord’s way of supporting me through this terrible time.”

Dr Palesa Monyake, paediatric intensivist at Netcare Waterfall City Hospital’s specialised PICU, is pictured with Hannah-Grace Hefer and her mother, Megan.
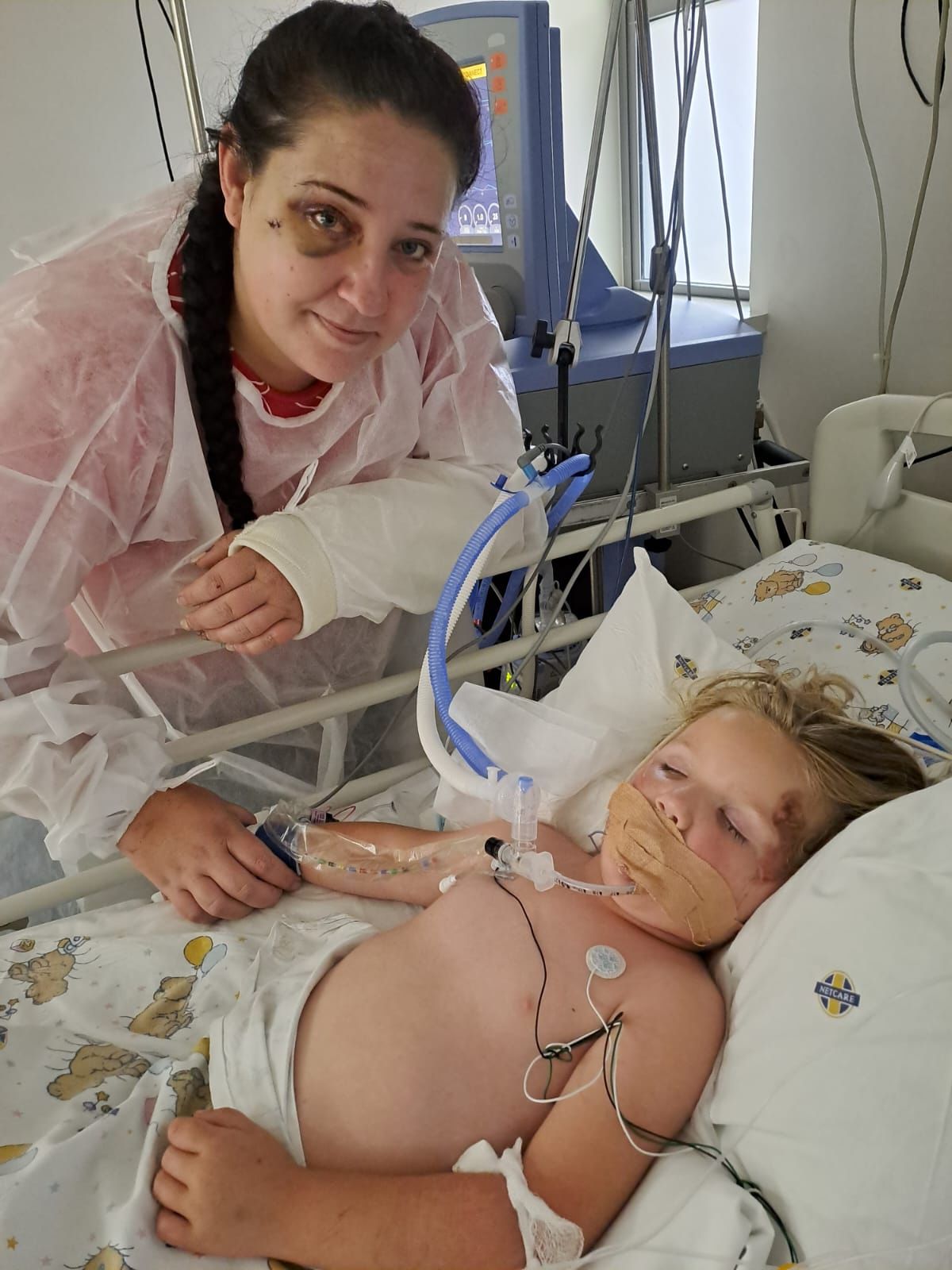
Megan Hefer reflects on her daughter’s progress ahead of World Head Injury Awareness Day on 20 March, following the family’s tragic car accident in early January.
WATCH: Hannah-Grace and Charne Cox: At Netcare Rehabilitation Hospital, Hannah-Grace learnt to walk again with the support of a multidisciplinary team, including physiotherapist Charne Cox. This video captures her milestone first steps after the accident.
At last, Hannah-Grace could breathe on her own, but the extent of the neurological effects remained unclear. Scans revealed areas of bleeding in Hannah-Grace’s brain, which can indicate damage to areas of the brain responsible for movement, language and other crucial functions.
“Her eyes were only staring to the right, but we didn’t know if she could see or hear. She didn’t talk, and she didn’t show any signs that she recognised me,” her mother remembers.
Megan, her mother, sister, Dr Monyake and the PICU nurses prayed for Hannah-Grace’s recovery. “As time went on, she started speaking a few words. One day, she said, ‘Ek is Hannah Grace,’ and she seemed to know herself for the first time. I cried out, ‘My baby is coming back’.”
Dr Monyake describes Hannah-Grace’s mother as “a pillar of strength,” whose love, support, and faith at her daughter’s bedside were invaluable. With Hannah-Grace medically stable at last, she was ready for the intensive therapies that would aid her recovery at Netcare Rehabilitation Hospital.
Dr Anrie Carstens, a general practitioner with a special interest in physical and rehabilitation medicine, said that when Hannah-Grace arrived, the most prominent feature of her injury was pronounced weakness on the left side of her body, in keeping with a stroke in the basal ganglia of the brain.
“Hannah-Grace’s brain had to relearn how to recognise the left side of her body so she could learn to walk again. When she came in, her expressive and receptive language skills were also delayed. Her initial assessment anticipated she would need eight weeks of intensive therapy at Netcare Rehabilitation Hospital, but she was so eager to get going with her therapy sessions and progressed so quickly that we were amazed when she needed less than half this time.”
According to Dr Carstens, brain injuries in children often have a greater potential to heal and regain lost functionality, provided there is prompt and appropriate emergency care, as well as the required specialised care after the injury, followed by neurologically informed intensive multidisciplinary therapy.
“The neuroplasticity of children’s brains means they often have the most to gain from rehabilitative therapies as soon as possible after injury. In Hannah-Grace’s case, although she was withdrawn at first, she grew in confidence and showed progress in important functional areas – engaging in symbolic play, initiating activities and improving her social skills. Most poignantly, she showed tender attentiveness and empathy for one of the children she befriended in the ward,” Dr Carstens says.
Given the trauma of the accident and the loss of her father, psychological support and play therapy were provided as part of the multidisciplinary care Hannah-Grace received at the hospital.
Physiotherapist Charne Cox helped Hannah-Grace develop her balance, coordination and mobility during her rehabilitation admission. “At first she couldn’t crawl or walk, but she tried so hard from the beginning that we could see she was going to do well. Every week, we realised she was making such rapid progress that she would not stay as long as we expected,” Cox says.
Making therapy fun and engaging is crucial for capturing children’s attention, and activities such as baking, making necklaces and movement games on a big screen TV featuring Hannah-Grace’s favourite cartoon characters were just some of the tools used in her therapy.
“Hannah Grace’s mom was a true champion, supporting her daughter every step of the way and helping to keep her attention focused on the therapy while also maintaining the boundaries of parenthood that can often be hard to maintain when a child has suffered a brain injury. She also asked the right questions to prepare for Hannah-Grace’s return to the home environment,” Cox says.
Dr Carstens says that after just three weeks at Netcare Rehabilitation Hospital, Hannah-Grace’s functional testing score rose dramatically. “She arrived with a score of 35 – far below the average of 91 for her age – but improved to 85. With additional fine-tuning and continued outpatient therapy, we fully expect Hannah-Grace to continue improving, just as she thrived during her time with us.”
Megan says that Hannah-Grace is making great strides – literally. Her walking is almost back to normal, she’s talking in both English and Afrikaans, and she’s spending time with Buddy, the Yorkshire terrier she and her late husband bought for their daughter for Christmas just before the accident.
“She is doing so well, and she is so eager to play and run around that I have my hands full trying to keep her from being a little gymnast. The doctors advised that another bump to the head could be serious for Hannah-Grace, so I have to remind her to be careful when she is playing.
“It was God’s grace that restored her to us, and now I fully realise the significance of why we named her Hannah-Grace. Every nurse, every doctor and therapist, every person who had a role in the miracle of her recovery and showed us such care and kept us in your prayers throughout, we are so grateful for each one of you,” Megan concludes.













